Bone and Tissue Regeneration A Game Changer
British researchers at the University of Birmingham conducted a study that could alter the field of regenerative medicine. They developed a way to regenerate human bone and tissue using nano-scale structures, helping the body more efficiently replace lost tissue. Although it will be many years before the technology is approved for public use, the implications of this research can significantly alter the use of stem cell therapy.
Advancements in Stem Cell Therapy
Global Stem Cells Group offers not only equipment and kits for point-of-care stem cell applications, but also through Stem Cells Training Inc, we provide physicians with hands-on stem cell training. This training is designed for those who want to get involved in this exciting field of medicine. Degenerative conditions could be better treated through the use of stem cell technology. To better understand what this technology entails, we will use osteoarthritis as a prime example.
Understanding Osteoarthritis and Stem Cell Therapy
In case you were unaware, osteoarthritis is a condition where the tissue between the joints starts to degrade, preventing the free movement of the joints. This can cause severe pain in sufferers of the condition. To help relieve the pain, the doctors attending our courses are taught to use the equipment for PRP and adipose-derived stem cells isolation and processing. The use of this technology can help reverse some of the effects, lower pain, and allow for more movement.
What Was Discovered in the Study
It was discovered by the researchers that these nano-structures could be produced naturally through the stimulation of human cells. These structures are known as vesicles, small extracellular structures that can have a multitude of functions, such as helping cells create certain substances.
Researchers concluded that “purifying” these vesicles could produce a substance highly beneficial in regenerative medicine. This could be used to create new growth tissue. The efforts were focused on making a tissue that can be used in more than one patient, as opposed to the more autologous method that current doctors are trained in.
Autologous vs. Allogeneic Treatments
Autologous treatment involves taking stem cells from the patient being treated and injecting them into the treatment area. This method lowers rejection rates, but each treatment requires new stem cells. The researchers at the University of Birmingham are exploring a new approach.
They aim to create a treatment that any patient can use. They believe that vesicles are important in this process and have shown that vesicles can be used to regenerate tissue regardless of the initial owner of the cells. This means that a single sample could potentially be used to treat multiple people.
Why This Matters
Regardless of the criticisms of stem cell research, ongoing research allows us to further train our doctors. This excites us as we strive to teach the best and most effective methods for our patients. This research helps us treat countless patients and makes significant strides in medical research, helping people worldwide seek treatment for various ailments.
Regenerative medicine has great potential. It can alter the landscape of modern healthcare, shifting it away from an era reliant on surgery and medications to treat every ailment. Regenerative medicine offers a promising alternative that will help treat and potentially cure diseases, rather than just managing symptoms.
Future Implications
Hopefully, this research will prove effective and be applicable to a wide range of diseases, potentially eliminating the need for various surgeries. This could also reduce the number of pharmaceuticals on the market. Over time, this treatment may help us create whole tissue in the lab.
- Published in Corporate News / Blog
IFATS Recommendations for FDA Regulation of Human Cells, Tissues, and Cellular and Tissue-Based Products
International Federation of Adipose Therapeutics and Sciences (IFATS)
45 Lyme Road – Suite 304
Hanover, NH 03755 USA
Tel: 1-603-643-2325
Fax: 1-603-643-1444
September 26, 2016
Division of Dockets Management (HFA–305)
Food and Drug Administration
5630 Fishers Lane, Rm. 1061
Rockville, MD 20852
Re: FDA-2014-D-1856 – Comments to 2014-2015 Draft Guidance
Docket FDA-2014-D-1584: “Same Surgical Procedure Exception under 21 CFR 1271.15(b): Questions and Answers Regarding the Scope of the Exception; Draft Guidance for Industry”;
Docket FDA-2014-D-1696: “Minimal Manipulation of Human Cells, Tissues, and Cellular and Tissue-Based Products; Draft Guidance for Industry and Food and Drug Administration Staff”;
Docket FDA-2014-D-1856: “Human Cells, Tissues, and Cellular and Tissue-Based Products from Adipose Tissue: Regulatory Considerations; Draft Guidance for Industry”;
Docket FDA-2015-D-3581: “Homologous Use of Human Cells, Tissues, and Cellular and Tissue-Based Products; Draft Guidance for Industry and FDA Staff.”
Dear Sirs and Madams:
The International Federation of Adipose Therapeutics and Sciences (IFATS) appreciates this opportunity to submit the following comments to supplement its earlier written comments and recent testimony at the September 12-13, 2016 Public Hearing on the 2014-2015 Draft HCT/P Guidances concerning: a) Minimal Manipulation; b) Same Surgical Procedure; c) Adipose Tissue; and d) Homologous Use.
IFATS is committed to the responsible advance of the science and translation of new adipose therapies and is determined to ensure patient safety. It was founded in 2003 by pioneering adipose stem cell biologists and clinician–scientists with the goal of advancing the science of adipose tissue biology and its clinical translation to therapeutic applications. Since that time, IFATS has remained at the forefront of regenerative medical applications involving adipose tissue and cells. Membership now spans 40 countries in North America, Europe, Africa, the Middle East, Asia, Australia, and Central and South America, and includes basic scientists, translational researchers, clinicians, and regulatory and biotech representatives. IFATS is formally aligned with, and its members serve on the editorial boards of the prestigious journals, Stem Cells and Stem Cells Translational Medicine. With the International Society for Cellular Therapy (ISCT), IFATS has provided the scientific community with a detailed description and definition of adipose-derived cells (both stromal vascular fraction, or SVF, and adipose-derived stromal/stem cells, or ASCs) in the formal publication entitled Cytotherapy. Thus, IFATS possesses the necessary expertise to assist regulatory agencies in understanding adipose tissue and regulating the safety and efficacy of adipose-related products and therapies.
Recommendations for FDA Regulation
Drawing on this expertise, IFATS has reviewed the four draft guidances with great care. It respectfully requests the FDA to reconsider and modify the four draft HCT/P guidances as follows:
Recommendation #1 – Cell-Based Risks
Interpret and evaluate an HCT/P’s homologous use and minimal manipulation based on its manufacturer’s intended use in the patient.
Recommendation #2 – Provider-Based Risks
Reduce provider-created risks by targeting provider behavior.
Recommendation #3 – Adipose HCT/P Functions
Recognize that adipose HCT/Ps have both structural and nonstructural functions, and regulate based on its manufacturer’s intended use in the patient.
Recommendation #4 – Evaluation of Minimal Manipulation and Homologous Use
Revise the evaluation of minimal manipulation and homologous use as they pertain to particular applications of adipose tissue.
IFATS recognizes the FDA’s challenge in developing regulations that fulfill the agency’s dual and interrelated responsibilities of protecting patients while promoting innovation. IFATS further recognizes that although these are complementary rather than competing objectives, they are often difficult to pursue simultaneously. The FDA’s three-tiered, risk-based §§ 361 – 351 framework balances these concerns by making the degree of regulatory oversight proportionate to the degree of an HCT/P therapy’s risk.
Key Concepts: Homologous Use and Minimal Manipulation
The concepts of homologous use and minimal manipulation are key determinants of whether an HCT/P will be classified as a § 361 product (which does not need premarket approval) or a § 351 drug, device, and/or biological product (which requires formal premarket approval). The applicability of § 351’s “same surgical procedure” exception also turns on homologous use and minimal manipulation. For most manufacturer-clinicians, § 351 categorization raises insurmountable obstacles due to the time and expense of obtaining premarket approval. In such cases, § 351 classification effectively prohibits access to safe and effective HCT/P therapies, even when those therapies involve a patient’s own cells and/or can deliver superior results with reduced risks. At the same time, § 351 oversight is essential for therapies that pose greater risks due to the HCT/P’s characteristics, mechanisms of action, and circumstances of use.
Addressing Provider Misconduct
A second type of risk involves rogue clinicians offering false promises in the form of unproven therapies performed with few safeguards and less training. Provider misconduct is not unique to HCT/P therapies; it pervades all areas of medical practice. Nevertheless, IFATS shares the FDA’s alarm over such practices in the context of HCT/Ps, and is equally determined to curtail them. Because a solution cannot solve a problem without identifying and attacking its root cause, effective regulation of HCT/P-related risks must recognize and respond to their multivariate causes.
Put simply:
Sections 351 and 361 in Regulating HCT/P Therapies
Sections 351 and 361 appropriately attempt to regulate HCT/P therapies proportionate to the risks of unpredictable and/or unsafe cell behavior. However, the risks of untrained providers misusing HCT/P therapies are caused by providers misbehaving, not cells misbehaving. Consequently, interpretive guidance that restricts the definition and application of HCT/P terminology can only go so far in restricting provider-based risks. In addition, restrictive, inaccurate, or imprecise definitions and interpretations carry their own risks of restricting access to therapies and restricting a patient’s right to evaluate risk through the process of informed consent.
A Two-Part Strategy for Regulating HCT/P Risks
Therefore, IFATS recommends that the FDA adopt an overall two-part strategy that focuses on both categories of HCT/P risks, i.e., those relating to cell behavior and those that pertain to provider behavior.
Recommendation #1 – Cell-Based Risks
Interpret and evaluate an HCT/P’s homologous use and minimal manipulation based on its manufacturer’s intended use in the patient. Interpretive guidance should predicate each definition on the functions and/or characteristics of the specific composition (i.e., cell type(s) and/or matrix or other component(s)) that are involved in, and/or relevant to the manufacturer-clinician’s intended use in the patient.
Recommendation #2 – Provider-Based Risks
To reduce provider-created risks, the FDA should target provider behavior by collaborating with IFATS and comparable organizations to draw on and supplement existing federal and state methods of certification, registration, and similar measures.
The Benefits of a Two-Part Strategy
Adopting this two-part strategy can control risk more comprehensively – and therefore more effectively – in furtherance of the FDA’s dual and interrelated obligations of protecting patients and promoting the availability of HCT/P therapies. IFATS explains each recommendation as follows:
Detailed Explanation of Recommendation #1 – Cell-Based Risks
Interpret and evaluate an HCT/P’s homologous use and minimal manipulation based on its manufacturer’s intended use in the patient. The four draft guidances on homologous use, minimal manipulation, same surgical procedure, and adipose tissue individually and collectively intend to “improve stakeholders’ understanding” of 21 CFR 1271 by clarifying the FDA’s interpretation of homologous use and minimal manipulation. As demonstrated by the initial round of public comments and the ensuing public hearing on September 12 and 13, 2016, the draft guidance documents have not clarified applicable regulations. They have instead compounded the difficulty of understanding and complying with them. The drafts’ introduction of new definitional inaccuracies has also amplified rather than reduced patient risk.
IFATS respectfully requests the agency to clarify the definitions and application of homologous use and minimal manipulation by interpreting each as referring to the characteristics of the specific cell type(s) and/or the matrix or other component(s) that are involved in, and/or relevant to the manufacturer’s intended use in the patient. Thus, the definition of homologous use with interpretive guidance would read as follows:
21 CFR 1271.3(c): Homologous use means the repair, reconstruction, replacement, or supplementation of a recipient’s cells or tissues with an HCT/P that performs the same basic function or functions in the recipient as in the donor.
Recommended GUIDANCE: As used in this section, “performs the same basic function or functions in the recipient as in the donor” shall be interpreted as referring to one or more of the function(s) of the specific composition of the therapeutic/product, reflecting the specific cell type(s) and/or the specific matrix or other component(s) in the donor tissue that are involved in, and/or relevant to the manufacturer’s intended use in the patient.
Similarly, the definition of minimal manipulation with interpretive guidance would read as follows:
21 CFR 1271.3(f) Minimal manipulation means:
- For structural tissue, processing that does not alter the original relevant characteristics of the tissue relating to the tissue’s utility for reconstruction, repair, or replacement;
- For cells or nonstructural tissues, processing that does not alter the relevant biological characteristics of cells or tissues.
Recommended GUIDANCE: As used in this section, “relevant” characteristics shall be interpreted to mean the characteristics of the specific cell type(s) and/or the specific matrix or other component(s) in the donor tissue that are involved in, and/or relevant to the manufacturer’s intended use in the patient.
Rationale for Recommendations
Incorporating and relying on the manufacturer’s intended use harmonizes the interpretation and definition of homologous use and minimal manipulation with statutory directives to predicate the regulation of drugs, devices, and biologics on the manufacturer’s intended use. Defining relevant characteristics in terms of “the characteristics of specific cell type(s) and/or the matrix or other component(s) in the donor tissue that are involved in, and/or relevant to the manufacturer’s intended use in the patient” promotes patient safety by insisting on a reasonable and scientifically supportable rationale for using an HCT/P for a particular mechanism of action. This clarification balances the FDA’s dual responsibilities of protecting patients from undue safety risks while promoting the ongoing availability and continued development of HCT/P therapies.
Example of Non-Homologous Use: Decellularized adipose matrix used to accomplish the manufacturer’s intended use of a particular metabolic or systemic effect in the patient (e.g., reducing insulin levels in a diabetic patient) is non-homologous because decellularized matrix is not relevant to metabolic or systemic activity.
Here’s an improved version of your article with added H2 headings for better on-page SEO and readability:
Recommendation #2 – Provider-Based Risks
Targeting Provider Behavior
To reduce provider-created risks, the FDA should target provider behavior by collaborating with IFATS and comparable organizations to draw on and supplement existing federal and state methods of certification, registration, and similar measures. For a risk-reduction strategy to succeed, it must target the root cause of the risk. Revising, retracting, or replacing interpretations of regulatory terminology can target the risks of cells behaving in unsafe ways but can do little to prevent providers from behaving in unsafe ways.
Existing Mechanisms for Provider Oversight
Because the risks of irresponsible providers offering unsafe treatments are not exclusive to HCT/P therapies, many federal and state mechanisms already exist for identifying, disciplining, and prohibiting clinics and clinicians from endangering patients. IFATS shares the FDA’s concern about provider-related risks in the HCT/P sector and shares its determination to end or minimize these risks. IFATS respectfully requests the FDA to collaborate with it and comparable organizations to identify and draw on existing federal and state methods for curtailing provider misconduct and developing additional protections in the form of provider certification, registration, monitoring, and similar measures.
The Need for Collaboration
At present, the §§ 351-361 regulatory framework does not – and cannot – adequately respond to this form of risk. Collaboration among stakeholders and coordination with existing means of provider oversight offers the most effective and efficient strategy for protecting patients from provider-created risk. Therefore, IFATS respectfully requests the FDA to meet with IFATS, the American Association of Blood Banks, and other accreditation bodies to work together to identify provider-focused safety objectives and measures that can be translated into formal accreditation requirements and interpretive guidance.
Recommendation #3: Recognize Structural and Nonstructural Functions of Adipose HCT/Ps
Expanding the Definition of Adipose Tissue
IFATS requests the FDA to expand its definition of adipose tissue from exclusively structural in function to include both structural and/or nonstructural functions, depending on the manufacturer’s intended use in the patient. This modification is critically necessary to:
- Reconcile the interpretive guidance on the definition and regulation of adipose with applicable statutory and regulatory requirements.
- Reflect and ensure biological accuracy.
- Regulate an HCT/P’s risks based on the manufacturer’s intended use and mechanisms of action in the patient.
Statutory and Regulatory Requirements
Structural and Nonstructural Functions
Recognizing adipose tissue’s structural and/or nonstructural functions is required by applicable statutory and regulatory requirements. Adipose HCT/Ps must be defined as having structural and/or nonstructural functions to align the draft guidance with statutory and regulatory recognition that cells and tissues may have more than one function. According to 42 USC § 321(g)(1):
“[t]he term ‘drug’ means … (B) articles intended for use in the diagnosis, cure, mitigation, treatment, or prevention of disease in man or other animals; and (C) articles (other than food) intended to affect the structure or any function of the body of man or other animals; and (D) articles intended for use as a component of any article specified in clause (A), (B), or (C).”
Statutory directives to focus on intended use pervade FDA regulation, including the regulation of drugs, biologics, devices, cosmetics, pesticides, and more. Applicable statutes and regulations explicitly and implicitly recognize that the human body is complex, and its tissues and cells are often versatile and multi-functional. For example, 21 CFR 1271.3(c)’s definition of homologous use correctly recognizes that an HCT/P may have more than one “basic function.” It never says or even suggests that an HCT/P can only have one function or that the regulator has sole authority to define that function and thereby dictate a manufacturer’s intended use. And yet the draft guidances do just that by insisting that adipose HCT/Ps are solely structural.
Correcting Factual Inaccuracy
The Complexity of Adipose Tissue
Recognizing adipose tissue’s structural and/or nonstructural functions is necessary to correct factual inaccuracy. Regulation 21 CFR 1271.10(a)(4) categorizes an HCT/P as “either” structural or nonstructural, depending on its function. A structural HCT/P “does not have a systemic effect and is not dependent upon the metabolic activity of living cells for its primary function.” A nonstructural HCT/P “has a systemic effect or is dependent upon the metabolic activity of living cells for its primary function.”
The draft adipose guidance expressly acknowledges that adipose tissue contains adipocytes, preadipocytes, fibroblasts, vascular endothelial cells, a variety of immune cells, and also stores energy in the form of lipids. Citing only Junqueira’s Basic Histology: Text & Atlas, the draft guidance classifies adipose as connective and therefore structural tissue. This result is internally inconsistent and factually inaccurate – and the FDA’s sole cited authority explains why.
Adipose Tissue as Specialized Connective Tissue
Junqueira classifies connective tissue as: 1) connective tissue proper; 2) embryonic connective tissues; and 3) specialized connective tissues. The latter category defines specialized connective based on their principal specialized functions. Blood, reticular connective tissue, adipose tissue, bone, and cartilage all qualify as specialized connective tissues with specialized, nonstructural functions. Junqueira’s examples include the following:
- Blood is a specialized connective tissue; its principal function of transport is nonstructural.
- Reticular connective tissues include the liver, pancreas, bone marrow, and lymph nodes. They are nonstructural tissues because their principal functions are metabolic, including endocrine.
According to Junqueira – the FDA’s sole cited authority – adipose tissue is nonstructural specialized connective tissue; its primary function is metabolic with co-existing structural functions.
Historical and Scientific Consensus
Junqueira’s categorization of adipose as primarily nonstructural reflects longstanding scientific consensus. In 1893, Gustav Neuber described his use of fat grafting in the orbital region to heal the adherent scarring which was the sequela of osteomyelitis. As a result of its nonstructural healing functions, the fat graft transformed facial scarring to more normal-appearing skin and subcutaneous tissues. In 1912, Holländer described the successful use of fat injections to prevent the recurrence of scarring following breast surgery. In 1926, Charles Conrad Miller developed a new system for injecting fat grafts and described 36 cases of correcting cicatricial contraction on the face and neck and reported “excellent results” for another 2 cases after using fat grafts to treat “very persistent parotid fistulas…which defied all other methods of treatment.” These and similarly favorable outcomes resulted from fat’s transformational nonstructural repair of the tissues into which it was placed.
Adipose Tissue as an Endocrine Organ
The understanding of the diverse roles of adipose tissue has steadily expanded due in large part to the discovery of the first widely accepted adipokine, leptin, in the mid-1990s. Adipose tissue secretes proteins with systemic actions on hematopoietic, reproductive, metabolic, and other cells and tissues, demonstrating unequivocally that adipose meets the definition of a true “endocrine” organ.
Research and Scientific Evidence
A Google Scholar search of all available online medical and research databases for “the primary function of Adipose Tissue” returns 538,000 journal articles. Although the search did not designate a specific function, the search results referred to adipose tissue almost exclusively as a nonstructural metabolic and endocrine organ with secretory properties. A search for an exact match of the phrase “primary function of adipose tissue” yielded the following: “It was long believed the primary function of adipose tissue was energy storage; in fact, stromal adipose is a complicated endocrine organ.” However, even energy storage is nonstructural.
FDA’s Draft Guidance on Minimal Manipulation
The FDA’s draft guidance on minimal manipulation defines nonstructural tissues as “serv[ing] predominantly metabolic or other biochemical roles in the body such as hematopoietic, immune, and endocrine functions.” To illustrate, the draft guidance offers “cord blood, lymph nodes, pancreatic tissue” as examples of nonstructural tissue. These tissues are indeed nonstructural – but they are also specialized connective tissue, as explained in Junqueira. In addition, adipose has “hematopoietic, immune, and endocrine functions,” as explained below. As demonstrated by Junqueira, adipose HCT/Ps clearly do more than “reconstruction, repair, or replacement that relate to its utility to cushion and support the other tissues in the subcutaneous layer (subcutaneum) and skin.” And the FDA’s own nonstructural examples prove that classifying connective tissue, including adipose tissue as solely structural, is factually inaccurate and logically flawed.
IFATS’ Recommendation
Thus, IFATS strongly recommends that the draft guidances be revised to define and categorize adipose tissue as having both structural and nonstructural functions. In support, IFATS offers the following examples of adipose’s nonstructural, and combined nonstructural and structural functions.
Nonstructural Functions of Adipose HCT/Ps
Nonstructural Endocrine Functions
It is well recognized that adipose is an endocrine organ which, like other endocrine organs, performs a variety of nonstructural functions. Adipose tissue secretes proteins with nonstructural, systemic actions on hematopoietic, reproductive, metabolic, and other cells and tissues.
Recommendation #2 – Provider-Based Risks
To reduce provider-created risks, the FDA should target provider behavior by collaborating with IFATS and comparable organizations to draw on and supplement existing federal and state methods of certification, registration, and similar measures.
For a risk-reduction strategy to succeed, it must target the root cause of the risk. Revising, retracting, or replacing interpretations of regulatory terminology can target the risks of cells behaving in unsafe ways but can do little to prevent providers from behaving unsafely. Many federal and state mechanisms already exist for identifying, disciplining, and prohibiting clinics and clinicians from endangering patients, as the risks of irresponsible providers offering unsafe treatments are not exclusive to HCT/P therapies.
IFATS shares the FDA’s concern about provider-related risks in the HCT/P sector and is determined to end or minimize these risks. IFATS respectfully requests the FDA to collaborate with it and comparable organizations to identify and draw on existing federal and state methods for curtailing provider misconduct and developing additional protections in the form of provider certification, registration, monitoring, and similar measures. At present, the §§ 351-361 regulatory framework does not – and cannot – adequately respond to this form of risk. Collaboration among stakeholders and coordination with existing means of provider oversight offer the most effective and efficient strategy for protecting patients from provider-created risk.
Therefore, IFATS respectfully requests the FDA to meet with IFATS, the American Association of Blood Banks, and other accreditation bodies to identify provider-focused safety objectives and measures that can be translated into formal accreditation requirements and interpretive guidance.
Recommendation #3: Recognize that Adipose HCT/Ps Have Both Structural and Nonstructural Functions
IFATS requests the FDA to expand its definition of adipose tissue from exclusively structural in function to include both structural and/or nonstructural functions, depending on the manufacturer’s intended use in the patient. This modification is critically necessary to:
- Reconcile the interpretive guidance on the definition and regulation of adipose with applicable statutory and regulatory requirements;
- Reflect and ensure biological accuracy; and most importantly,
- Regulate an HCT/P’s risks based on the manufacturer’s intended use and mechanisms of action in the patient.
Adipose Tissue’s Structural and Nonstructural Functions
a. Recognizing Adipose Tissue’s Structural and/or Nonstructural Functions is Required by Applicable Statutory and Regulatory Requirements
Adipose HCT/Ps must be defined as having structural and/or nonstructural functions to align the draft guidance with statutory and regulatory recognition that cells and tissues may have more than one function. According to 42 USC § 321(g)(1), “[t]he term ‘drug’ means … (B) articles intended for use in the diagnosis, cure, mitigation, treatment, or prevention of disease in man or other animals; and (C) articles (other than food) intended to affect the structure or any function of the body of man or other animals; and (D) articles intended for use as a component of any article specified in clause (A), (B), or (C). (emphasis added). Statutory directives to focus on intended use pervade FDA regulation, including the regulation of drugs, biologics, devices, cosmetics, pesticides, and more. Applicable statutes and regulations explicitly and implicitly recognize that the human body is complex, and its tissues and cells are often versatile and multifunctional. For example, 21 CFR 1271.3(c)’s definition of homologous use correctly recognizes that an HCT/P may have more than one “basic function.” It never says or even suggests that an HCT/P can only have one function, or that the regulator has sole authority to define that function and thereby dictate a manufacturer’s intended use. And yet the draft guidances do just that by insisting that adipose HCT/Ps are solely structural.
To align interpretive guidance with the regulations and statutory provisions being interpreted, IFATS respectfully requests the FDA to avoid pre-determining specific functions and uses for specific HCT/Ps. Instead, it should base regulations and guidance on the HCT/P’s function(s) and characteristic(s) relevant to its intended use by the manufacturer.
b. Recognizing Adipose Tissue’s Structural and/or Nonstructural Functions is Necessary to Correct Factual Inaccuracy
Regulation 21 CFR 1271.10(a)(4) categorizes an HCT/P as “either” structural or nonstructural, depending on its function. A structural HCT/P “does not have a systemic effect and is not dependent upon the metabolic activity of living cells for its primary function.” A nonstructural HCT/P “has a systemic effect or is dependent upon the metabolic activity of living cells for its primary function.”
The draft adipose guidance expressly acknowledges that adipose tissue contains adipocytes, preadipocytes, fibroblasts, vascular endothelial cells, a variety of immune cells, and also stores energy in the form of lipids. Citing only Junqueira’s Basic Histology: Text & Atlas, the draft guidance classifies adipose as connective and therefore structural tissue. This result is internally inconsistent and factually inaccurate – and the FDA’s sole cited authority explains why.
Junqueira classifies connective tissue as 1) connective tissue proper; 2) embryonic connective tissues; and 3) specialized connective tissues. The latter category defines specialized connective based on their principal specialized functions. Blood, reticular connective tissue, adipose tissue, bone, and cartilage all qualify as specialized connective tissues with specialized, nonstructural functions. Junqueira’s examples include the following:
- Blood is a specialized connective tissue; its principal function of transport is nonstructural.
- Reticular connective tissues include the liver, pancreas, bone marrow, and lymph. They are nonstructural tissues because their principal functions are metabolic, including endocrine.
According to Junqueira – the FDA’s sole cited authority – adipose tissue is nonstructural specialized connective tissue; its primary function is metabolic with co-existing structural roles.
Examples of Adipose Tissue Functions
1. Nonstructural Endocrine Functions
It is well recognized that adipose is an endocrine organ performing a variety of nonstructural functions. Adipose tissue secretes proteins with nonstructural, systemic actions on hematopoietic, reproductive, metabolic, and other cells and tissues.
- Glucose and lipid metabolism control via adipokine secretion
- Reproductive and endocrine control via adipokine secretion
- Immunomodulatory and immunosuppressive systemic control via cytokine and protein factor secretion
2. Nonstructural Paracrine Functions
- Angiogenic control via vasculogenic cytokine secretion
- Hematopoietic control via cytokine secretion, both locally and systemically
- Neurogenesis via secretion of cytokine factors
3. Nonstructural Hematopoietic Potential of Adipose Stem Cells
- Reservoir for hematopoietic and lymphoid progenitor cells similar to bone marrow
- Thermogenesis (brown and beige fat)
- Energy reservoir (white adipose depots)
4. Nonstructural Promotion of Lactation
- Fat serves as an energy reservoir and nutrient supply for breast epithelial cells.
- As pregnancy progresses, the breast epithelium proliferates in a branching manner to occupy the majority of the adjacent adipose tissue and
- At parturition, the epithelial cells draw on the lipid reserves of adipocytes within immediate proximity and secrete these nutrients into the milk available to the newborn infant during lactation.
- As long as the mother continues to breastfeed the infant, the epithelial cells remain viable and
- If suckling is discontinued for periods of 24 to 48 hours, the epithelial cells undergo rapid apoptosis, leaving pre-adipocytes and adipocytes as the predominant cells within the breast tissue.
- While the presence and organization of epithelial cells within the breast tissue provide it with a unique architecture, the mammary adipocytes themselves show remarkable similarity to adipocytes from elsewhere in the body. Thus, the mammary fat pad displays homology to other adipose tissue depots .
5. Nonstructural Regenerative Functions
- Local and circulating multipotent progenitor cells can repair and regenerate damaged tissues such as repairing irradiated skin, alleviating fibrotic changes, improving mobility and vitality, and repairing structures such as hair follicles and . Specific examples include:
- Modulation of scarring
- Treating old burn scars
- Release of adherent scarring/fasciotomies
- Modulation of scarring in primary cleft lip repair
Multipotent progenitor cells may be recruited for the repair and regeneration of ischemic damage induced by acute myocardial infarction . Adipose mesenchymal stem cells as progenitor cells in a perivascular position contribute to vascular network formation and vascular structures【49†
Recommendation #4: Revise the Evaluation of Minimal Manipulation and Homologous Use of Adipose Tissue
IFATS respectfully requests the FDA reconsider its evaluation of three particular applications of adipose tissue regarding homologous use and minimal manipulation, each of which is required for § 361 classification as well as § 351’s “same surgical procedure” exception. Specifically, IFATS requests the FDA to revise its prior examples to recognize the following:
Decellularizing Adipose Tissue for Structural Use is Minimal Manipulation
The draft guidance currently states that decellularizing structural adipose tissue constitutes more than minimal manipulation because the process alters the tissue’s ability to perform structural functions. This is incorrect. Adipose tissue’s structural functions are performed by a dense and interconnected skeleton of reticular fiber and dense connective tissue. Its biomechanical properties include tensile strength and elasticity, both of which are central to the structural functions of padding and cushioning.
Nonstructural components such as adipocytes, pre-adipocytes, and lipids do not contribute to adipose’s structural characteristics or functions. It is well recognized that decellularization leaves adipose’s structural components fully intact. It does not alter, disturb, or weaken the remaining reticular fiber and dense connective tissue skeleton, or compromise its ability to perform structural functions. Multiple reports have demonstrated that decellularized adipose tissue retains structural properties and can be injected to impart padding and cushioning of soft tissues .
The FDA already classifies decellularized dermis as minimally manipulated, thereby acknowledging that the process of decellularization does not alter structural characteristics or functions of the remaining structural matrix. Removing cells from dermis and removing cells from adipose employ comparable methods to achieve comparable results. Decellularizing adipose for structural use, like decellularizing dermis for structural use, does not alter structural characteristics.
For these reasons, IFATS respectfully requests the FDA revise the draft guidance to recognize that decellularized adipose is minimally manipulated as required by § 361 and § 351’s “same surgical procedure” exception.
Structural Use of Fat in the Breast Constitutes Homologous Use
Example B-3 of the draft adipose guidance states that application of adipose-based HCT/Ps to the breast is nonhomologous use because “[t]he basic function of breast tissue is to produce milk (lactation) after childbirth. Because this is not a basic function of adipose tissue, using HCT/Ps from adipose tissues for breast augmentation would generally be considered a non-homologous use.” This logic is flawed and must be corrected because it mischaracterizes the function of the breast, and mischaracterizes the function of adipose in breast surgery.
For the purpose of determining homologous use, the basic function of the breast is as a secondary sex organ. In terms of shape, form, and appearance, the breast is vital to a woman’s bodily integrity and body image, psychological sense of self, and overall physical and emotional health and well-being. Lactation is not the sole or even primary function of the breast.
- Most women never lactate, but their breasts do function as secondary sex organs throughout their adolescence and adulthood.
- When lactation does occur, it is episodic, time-limited, and accounts for a very small fraction of a woman’s lifespan.
- Even when healthy, post-menopausal women cannot lactate. Restoring lactation is thus completely irrelevant to restoring breast function.
- All men have breasts, thousands develop breast cancer each year, and many will need reconstructive surgery — even though men do not lactate.
Federal law recognizes and protects the breast’s importance as a secondary sex organ. The Women’s Health and Cancer Rights Act, 29 USC 1185b(a), requires group health insurers to cover “all stages” of breast reconstruction following mastectomy or irradiation, including bilateral correction of asymmetrical appearance where one breast is otherwise unaffected. Restoring lactation is not a goal or even a remote concern of this statute. In fact, lactation is never mentioned in the statute’s text, legislative history, or associated regulations.
The function of adipose tissue in breast surgery is structural and therefore homologous.
Mastectomy removes more than the ability to lactate. It removes size, shape, and form by removing the breast mound, which is predominantly adipose. Consequently, applying adipose tissue for the structural purpose of restoring form and shape is homologous use. By classifying adipose-based tissues as non-homologous when applied to the breast, an entire class of Centers for Medicare & Medicaid Services (CMS) approved breast reconstruction procedures would be at risk for not complying with the same surgical procedure exception. For example:
- Autologous free tissue flap transfer (“free flap” breast reconstruction) is performed by transferring complex musculocutaneous flaps containing adipose tissue. One of the most common methods of reconstruction, it qualifies as an HCT/P because it completely removes fat-containing tissue flaps from the body before implanting .
- Fat grafting for breast reconstruction is another common clinical practice.
According to the draft adipose guidance, these and other methods of breast reconstruction could no longer be used without formal premarket approval because they do not restore lactation and are therefore non-homologous. Focusing solely on the restoration of lactation ignores the fact that the breast is largely composed of fat tissue and its size, shape, and form can be reconstructed with fat. This and other methods of breast reconstruction will no longer be available for clinical use under § 361 or § 351’s same surgical procedure exception because they will not restore lactation.
Removing these and other reconstructive methods from clinical application has nothing to do with risk. It is instead a perverse outcome of insisting that breast reconstruction be evaluated for its ability to restore the breast’s minor and episodic function of lactation despite fat’s ability to restore the breast’s size, shape, and function as a secondary sex organ.
For these reasons, IFATS respectfully requests the FDA revise the draft HCT/P guidance documents to recognize that as applied to the breast, adipose tissue is homologous use because it performs the structural functions of restoring, repairing, or reforming size, form, and shape.
Stromal Vascular Fraction (SVF) Cells for Nonstructural Use
When intended for nonstructural use in the patient, stromal vascular fraction (SVF) cells should be evaluated as nonstructural when determining minimal manipulation and homologous use. The FDA’s draft adipose guidance expressly acknowledges that adipose tissue contains a variety of nonstructural components, including adipocytes, preadipocytes, fibroblasts, vascular endothelial cells, and various immune cells, which store energy in the form of lipids. These are nonstructural because the cells perform the same regenerative functions in vivo as they do in vitro and in animal models .
Nonstructural adipose HCT/Ps are readily available in the stromal vascular fraction (SVF). Stromal vascular fractionation of lipoaspirate (typically obtained through liposuction) can remove fat’s structural components, making nonstructural SVF cells available for nonstructural use in a patient. Just as removing nonstructural cells through decellularization does not alter the relevant structural characteristics or structural function of the remaining structural matrix, removing structural components does not alter the relevant nonstructural characteristics or nonstructural function of the remaining nonstructural SVF components.
This is minimal manipulation under 21 CFR 1271.3(f)(2) because extracting nonstructural cells or tissues from lipoaspirate “does not alter the relevant biological characteristics of cells or tissues.” Also, this is homologous use under 21 CFR 1271.3(c) because it uses lipoaspirate’s nonstructural HCT/Ps for “repair, reconstruction, replacement, or supplementation of a recipient’s cells or tissues with an HCT/P that performs the same basic function or functions in the recipient as in the donor.”
Examples: Nonstructural Adipose Tissue for Homologous Use
Homologous Use with No Manipulation:
Using liposuction aspirate to perform fat grafting/adipose tissue therapy for the intended use of reversing radiation damage in the breast—a nonstructural function—is homologous use. The structural side-effect of increasing volume may be a collateral benefit, but the intended use is still nonstructural tissue repair.
- Use is homologous because the HCT/P performs that same basic nonstructural function in both donor and recipient.
Homologous Use with Minimal Manipulation:
Using liposuction aspirate is indicated for the nonstructural function of reversing radiation damage in the neck without the volume gain of a fat graft. Separating nonstructural from structural components obtains nonstructural SVF cells for nonstructural use in the patient.
- Use is homologous because it is performing the intended nonstructural function of reversing radiation damage.
- Manipulation is minimal because processing does not alter relevant nonstructural biological characteristics.
Homologous Use with More Than Minimal Manipulation:
Using liposuction aspirate is indicated for the nonstructural function of reversing radiation damage in the intestines by catheter injection of nonstructural SVF. However, an adequate dose is difficult to obtain because the patient is cachectic (low body fat caused by caloric depletion from radiation enteritis). Culture expansion is considered as a means of increasing dose.
- Use is again homologous because SVF cells would perform the intended nonstructural function of reversing radiation damage.
- Manipulation is more than minimal because culture expansion of cells to yield a therapeutic dose alters relevant biological characteristics. SVF cells in their natural state do not engage in linear growth to create a homogeneous monoculture. Even tumors
IFATS’s Gratitude and Request for Continued Collaboration with the FDA
The members of IFATS are grateful for the FDA’s willingness to re-open and extend the period for public comments and allow additional time for the September 2016 public hearing on the 2014-2015 draft HCT/P guidances. As a multidisciplinary scientific society composed of adipose stem cell biologists and clinician–scientists, IFATS would greatly appreciate the opportunity to work with the FDA in meeting the challenges of regulating HCT/P therapies.
Request for Meeting with FDA Representatives
We respectfully request that representatives of the FDA, including the Director of CBER, meet with members of IFATS to discuss the issues addressed herein as well as others that pertain to the advancement and regulation of adipose-based therapies.
Respectfully Submitted on Behalf of IFATS
Adam J. Katz, MD, FACS
Chair, IFATS Regulatory Affairs Committee & IFATS Co-Founder
University of Florida College of Medicine
Professor
Director of Plastic Surgery Research, Laboratory of BioInnovation and Translational Therapeutics
Division of Plastic Surgery, Department of Surgery
IFATS Board of Directors
Bruce Bunnell, PhD
Tulane University / United States
Louis Casteilla, PhD
University of Toulouse / France
Sydney Coleman, MD
New York & Pittsburgh Universities / United States
Julie Fradette, PhD
Lavalle University / Canada
William Futrell, MD
Founders’ Board, University of Pittsburgh / United States
Marco Helder, PhD
VU University Medical Center Amsterdam / The Netherlands
Adam J. Katz, MD, FACS
Founders’ Board, University of Florida / United States
Ramon Llull, MD, PhD
Founders’ Board, University of Barcelona / Spain
Kacey Marra, PhD
University of Pittsburgh / United States
Ricardo Rodriguez, MD
President (2016), Private Practice / Johns Hopkins / United States
Peter Rubin, MD, FACS
Chair, Founders’ Board, Chairman of the Board
University of Pittsburgh / United States
Stuart K. Williams, PhD
University of Louisville / United States
Members-at-Large
Jeff Gimble, MD, PhD
Pennington Biomedical / United States
Keith March, MD, PhD
Indiana University / United States
REFERENCES
- Bourin P, Bunnell BA, Casteilla L, Dominici M, Katz AJ, March KL, Redl H, Rubin JP, Yoshimura K, Gimble Stromal cells from the adipose tissue-derived stromal vascular fraction and culture expanded adipose tissue-derived stromal/stem cells: A joint statement of the International Federation for Adipose Therapeutics and Science (IFATS) and the International Society for Cellular Therapy (ISCT). Cytotherapy. 2013;15:641-648
- Diaz-Flores L, Gutierrez R, Madrid JF, Varela H, Valladares F, Acosta E, Martin-Vasallo P, Diaz-Flores L, Pericytes. Morphofunction, interactions and pathology in a quiescent and activated mesenchymal cell niche. Histol Histopathol. 2009;24:909-969
- Gimble The function of adipocytes in the bone marrow stroma. The New Biologist. 1990;2:304-312
- Cawthorn WP, Scheller EL, Learman BS, Parlee SD, Simon BR, Mori H, Ning X, Bree AJ, Schell B, Broome Bone marrow adipose tissue is an endocrine organ that contributes to increased circulating adiponectin during caloric restriction. Cell metabolism. 2014;20:368-375
- Meunier P, Aaron J, Edouard C, VlGNON Osteoporosis and the replacement of cell populations of the marrow by adipose tissue: A quantitative study of 84 iliac bone biopsies. Clinical orthopaedics and related research. 1971;80:147-154
- N. Über die wiederanheilung vollstädig vom körper getrennter, die ganze fettschicht en- thaltender hautstucke. Zbl f Chir 1893;30:16-17
- Hollander E, Joseph Cosmetic surgery. Handbuch der Kosmetik. Leipzig, Germany: Veriag von Velt. 1912;688
- Miller Cannula implants and review of implantation technics in esthetic surgery: In two parts. Oak Press; 1926.
- Gimble JM Fat circadian biology. Journal of applied physiology. 2009;107:1629-1637
- Tartaglia LA, Dembski M, Weng X, Deng N, Culpepper J, Devos R, Richards GJ, Campfield LA, Clark FT, Deeds Identification and expression cloning of a leptin receptor, ob-r. Cell. 1995;83:1263-1271
- Salgado AJ, Gimble Secretome of mesenchymal stem/stromal cells in regenerative medicine.
Biochimie. 2013;95:2195
- Salgado AJ, Reis RL, Sousa N, Gimble Adipose tissue derived stem cells secretome: Soluble factors and their roles in regenerative medicine. Curr Stem Cell Res Ther. 2009
- Khan M, Joseph Adipose tissue and adipokines: The association with and application of adipokines in obesity. Scientifica. 2014;2014
- Vicennati V, Garelli S, Rinaldi E, Di Dalmazi G, Pagotto U, Pasquali Cross-talk between
adipose tissue and the hpa axis in obesity and overt hypercortisolemic states. Hormone molecular biology and clinical investigation. 2014;17:63-77
- Kargi AY, Iacobellis Adipose tissue and adrenal glands: Novel pathophysiological mechanisms and clinical applications. International journal of endocrinology. 2014;2014
- Maïmoun L, Georgopoulos NA, Sultan Endocrine disorders in adolescent and young female athletes: Impact on growth, menstrual cycles, and bone mass acquisition. The Journal of Clinical Endocrinology
& Metabolism. 2014;99:4037-4050
- McIntosh K, Zvonic S, Garrett S, Mitchell JB, Floyd ZE, Hammill L, Kloster A, Di Halvorsen Y, Ting JP,
Storms RW. The immunogenicity of human adipose‐derived cells: Temporal changes in vitro. Stem cells. 2006;24:1246-1253
- McIntosh KR, Frazier T, Rowan BG, Gimble Evolution and future prospects of adipose- derived immunomodulatory cell therapeutics. Expert review of clinical immunology. 2013;9:175-184
- McIntosh KR, Lopez MJ, Borneman JN, Spencer ND, Anderson PA, Gimble Immunogenicity of allogeneic adipose-derived stem cells in a rat spinal fusion model. Tissue Engineering Part A. 2009;15:2677-2686
- Mitchell JB, McIntosh K, Zvonic S, Garrett S, Floyd ZE, Kloster A, Di Halvorsen Y, Storms RW, Goh B, Kilroy G. Immunophenotype of human adipose‐derived cells: Temporal changes in stromal‐associated and stem cell–associated markers. Stem cells. 2006;24:376-385
- Gimble JM, Dorheim MA, Cheng Q, Medina K, Wang CS, Jones R, Koren E, Pietrangeli C, Kincade Adipogenesis in a murine bone marrow stromal cell line capable of supporting b lineage lymphocyte growth and proliferation: Biochemical and molecular characterization. European journal of immunology. 1990;20:379-387
- Frazier TP, McLachlan JB, Gimble JM, Tucker HA, Rowan Human adipose-derived stromal/stem cells induce functional cd4+ cd25+ foxp3+ cd127− regulatory t cells under low oxygen culture conditions. Stem cells and development. 2014;23:968-977
- Frazier TP, Gimble JM, Kheterpal I, Rowan Impact of low oxygen on the secretome of human adipose- derived stromal/stem cell primary cultures. Biochimie. 2013;95:2286-2296
- Miranville A, Heeschen C, Sengenes C, Curat C, Busse R, Bouloumie Improvement of postnatal neovascularization by human adipose tissue-derived stem cells. Circulation. 2004;110:349-355
- Rehman J, Traktuev D, Li J, Merfeld-Clauss S, Temm-Grove CJ, Bovenkerk JE, Pell CL, Johnstone BH, Considine RV, March Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation. 2004;109:1292-1298
- Planat-Benard V, Silvestre J-S, Cousin B, André M, Nibbelink M, Tamarat R, Clergue M, Manneville C, Saillan-Barreau C, Duriez Plasticity of human adipose lineage cells toward endothelial cells physiological and therapeutic perspectives. Circulation. 2004;109:656-663
- Kilroy GE, Foster SJ, Wu X, Ruiz J, Sherwood S, Heifetz A, Ludlow JW, Stricker DM, Potiny S, Green P, Halvorsen YD, Cheatham B, Storms RW, Gimble Cytokine profile of human adipose-derived stem cells: Expression of angiogenic, hematopoietic, and pro- inflammatory factors. J Cell Physiol. 2007;212:702-709
- Ribeiro CA, Fraga JS, Grãos M, Neves NM, Reis RL, Gimble JM, Sousa N, Salgado The secretome of stem cells isolated from the adipose tissue and wharton jelly acts differently on central nervous system derived cell populations. Stem Cell Res Ther. 2012;3:18
- Silva NA, Gimble JM, Sousa N, Reis RL, Salgado Combining adult stem cells and olfactory ensheathing cells: The secretome effect. Stem cells and development. 2013;22:1232-1240
- Cho YJ, Song HS, Bhang S, Lee S, Kang BG, Lee JC, An J, Cha CI, Nam DH, Kim. Therapeutic effects of human adipose stem cell‐conditioned medium on stroke. Journal of neuroscience research. 2012;90:1794-1802
- Egashira Y, Sugitani S, Suzuki Y, Mishiro K, Tsuruma K, Shimazawa M, Yoshimura S, Iwama T, Hara The conditioned medium of murine and human adipose-derived stem cells exerts neuroprotective effects against experimental stroke model. Brain research. 2012;1461:87-95
- Wei X, Du Z, Zhao L, Feng D, Wei G, He Y, Tan J, Lee WH, Hampel H, Dodel Ifats collection:The conditioned media of adipose stromal cells protect against hypoxia‐ischemia‐induced brain damage in neonatal rats. Stem Cells. 2009;27:478-488
- Wei X, Zhao L, Zhong J, Gu H, Feng D, Johnstone B, March K, Farlow M, Du Adipose stromal cells-secreted neuroprotective media against neuronal apoptosis. Neuroscience letters. 2009;462:76-79
- Zhao L, Wei X, Ma Z, Feng D, Tu P, Johnstone B, March K, Du Adipose stromal cells- conditional medium protected glutamate-induced cgns neuronal death by bdnf. Neuroscience letters. 2009;452:238-240
- Cousin B, André M, Arnaud E, Pénicaud L, Casteilla Reconstitution of lethally irradiated mice by cells isolated from adipose tissue. Biochemical and biophysical research communications. 2003;301:1016-1022
- Han J, Koh YJ, Moon HR, Ryoo HG, Cho CH, Kim I, Koh Adipose tissue is an extramedullary reservoir for functional hematopoietic stem and progenitor cells. Blood.2009
- Harms M, Seale Brown and beige fat: Development, function and therapeutic potential. Nature medicine. 2013;19:1252-1263
- Rahman S, Lu Y, Czernik PJ, Rosen CJ, Enerback S, Lecka-Czernik Inducible brown adipose tissue, or beige fat, is anabolic for the skeleton. Endocrinology. 2013;154:2687-2701
- Wu J, Cohen P, Spiegelman Adaptive thermogenesis in adipocytes: Is beige the new brown? Genes & development. 2013;27:234-250
- Krings A, Rahman S, Huang S, Lu Y, Czernik P, Lecka-Czernik Bone marrow fat has brown adipose tissue characteristics, which are attenuated with aging and diabetes. Bone. 2012;50:546-552
- van Marken Lichtenbelt WD, Vanhommerig JW, Smulders NM, Drossaerts JM, Kemerink GJ, Bouvy ND, Schrauwen P, Teule Cold-activated brown adipose tissue in healthy men. N Engl J Med. 2009;360:1500-1508
- Peirce V, Carobbio S, Vidal-Puig The different shades of fat. Nature. 2014;510:76-83
- Enerbäck S, Gimble Lipoprotein lipase gene expression: Physiological regulators at the transcriptional and post-transcriptional level. Biochimica et Biophysica Acta (BBA)- Lipids and Lipid Metabolism. 1993;1169:107-125
- Rudolph MC, Neville MC, Anderson Lipid synthesis in lactation: Diet and the fatty acid switch. Journal of mammary gland biology and neoplasia. 2007;12:269-281
- Gimble JM, Katz AJ, Bunnell Adipose-derived stem cells for regenerative medicine. Circ Res. 2007;100:1249-1260
- Bellows CF, Zhang Y, Chen J, Frazier ML, Kolonin Circulation of progenitor cells in obese and lean colorectal cancer patients. Cancer Epidemiology Biomarkers & Prevention. 2011;20:2461- 2468
- Bellows CF, Zhang Y, Simmons PJ, Khalsa AS, Kolonin Influence of bmi on level of circulating progenitor cells. Obesity. 2011;19:1722-1726
- Krijnen PA NB, Meinster E, Vo K, Musters RJ, Kamp O, Niessen HW,, Juffermans LJ. Acute myocardial infarction does not affect functional characteristics of adipose derived stem cells in rats, but reduces the number of stem cells in adipose tissue. IFATS Annual Meeting. 2014:100
- Traktuev DO, Merfeld-Clauss S, Li J, Kolonin M, Arap W, Pasqualini R, Johnstone BH,March KL. A population of multipotent cd34-positive adipose stromal cells share pericyte and mesenchymal surface markers, reside in a periendothelial location, and stabilize endothelial networks. Circulation research. 2008;102:77-85
- Traktuev DO, Prater DN, Merfeld-Clauss S, Sanjeevaiah AR, Saadatzadeh MR, Murphy M, Johnstone BH, Ingram DA, March Robust functional vascular network formation in vivo by cooperation of adipose progenitor and endothelial cells. Circulation research. 2009;104:1410-1420
- Merfeld-Clauss S, Gollahalli N, March KL, Traktuev Adipose tissue progenitor cells directly interact with endothelial cells to induce vascular network formation. Tissue Engineering Part A. 2010;16:2953-2966
- Merfeld-Clauss S, Lupov IP, Lu H, Feng D, Compton-Craig P, March KL, Traktuev. Adipose stromal cells differentiate along a smooth muscle lineage pathway upon endothelial cell contact via induction of activin a. Circulation research. 2014;115:800-809
- Crisan M, Yap S, Casteilla L, Chen C-W, Corselli M, Park TS, Andriolo G, Sun B, Zheng B, Zhang A perivascular origin for mesenchymal stem cells in multiple human organs. Cell stem cell. 2008;3:301-313
- Ter Horst E, Naaijkens B, Krijnen P, Van Der Laan A, Piek J, Niessen Induction of a monocyte/macrophage phenotype switch by mesenchymal stem cells might contribute to improved infarct healing postacute myocardial infarction. Minerva cardioangiologica. 2013;61:617-625
- Guisantes E, Fontdevila J, Rodríguez Autologous fat grafting for correction of unaesthetic scars. Annals of plastic surgery. 2012;69:550-554
- Klinger M, Caviggioli F, Klinger FM, Giannasi S, Bandi V, Banzatti B, Forcellini D, Maione L, Catania B, Vinci Autologous fat graft in scar treatment. Journal of Craniofacial Surgery. 2013;24:1610-1615
- Klinger M, Marazzi M, Vigo D, Torre Fat injection for cases of severe burn outcomes: A new perspective of scar remodeling and reduction. Aesthetic plastic surgery. 2008;32:465-469
- Khouri RK, Smit JM, Cardoso E, Pallua N, Lantieri L, Mathijssen IM, Khouri Jr RK, Rigotti Percutaneous aponeurotomy and lipofilling: A regenerative alternative to flap reconstruction? Plastic and reconstructive surgery. 2013;132:1280-1290
- Balkin DM, Samra S, Steinbacher Immediate fat grafting in primary cleft lip repair. Journal of Plastic, Reconstructive & Aesthetic Surgery. 2014;67:1644-1650
- Rigotti G, Marchi A, Galie M, Baroni G, Benati D, Krampera M, Pasini A, Sbarbati. Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: A healing process mediated by adipose-derived adult stem cells. Plastic and reconstructive surgery. 2007;119:1409-1422
- Villani F, Caviggioli F, Klinger F, Klinger Rehabilitation of irradiated head and neck tissues by autologous fat transplantation. Plastic and reconstructive surgery. 2009;124:2190-2191
- Chang CC, Thanik VD, Lerman OZ, Saadeh PB, Warren SM, Coleman SR, Hazen Treatment of radiation skin damage with coleman fat grafting. STEM CELLS. 2007;25:3280-3281
- Sultan SM, Stern CS, Allen Jr RJ, Thanik VD, Chang CC, Nguyen PD, Canizares O, Szpalski C, Saadeh PB, Warren Human fat grafting alleviates radiation skin damage in a murine model. Plastic and reconstructive surgery. 2011;128:363-372
- Loder S, Peterson JR, Agarwal S, Eboda O, Brownley C, DeLaRosa S, Ranganathan K, Cederna P, Wang SC, Levi Wound healing after thermal injury is improved by fat and adipose-derived stem cell isografts. Journal of Burn Care & Research. 2015;36:70-76
- Sultan SM, Barr JS, Butala P, Davidson EH, Weinstein AL, Knobel D, Saadeh PB, Warren SM, Coleman SR, Hazen Fat grafting accelerates revascularisation and decreases fibrosis following thermal injury. Journal of Plastic, Reconstructive & Aesthetic Surgery. 2012;65:219-227
- Cuomo R, Zerini I, Botteri G, Barberi L, Nisi G, D’ANIELLO Postsurgical pain related to breast implant: Reduction with lipofilling procedure. In Vivo. 2014;28:993-996
- Maione L, Vinci V, Caviggioli F, Klinger F, Banzatti B, Catania B, Lisa A, Klinger Autologous fat graft in postmastectomy pain syndrome following breast conservative surgery and radiotherapy. Aesthetic plastic surgery. 2014;38:528-532
- Caviggioli F, Maione L, Forcellini D, Klinger F, Klinger Autologous fat graft in postmastectomy pain syndrome. Plastic and reconstructive surgery. 2011;128:349-352
- Caviggioli F, Vinci V, Codolini Autologous fat grafting: An innovative solution for the treatment of post-mastectomy pain syndrome. Breast Cancer. 2013;20:281-282
- Salgarello M, Visconti The role of sacrolumbar fat grafting in the treatment of spinal fusion instrumentation-related chronic low back pain: A preliminary report. Spine. 2014;39:E360-E362
- Faroni A, Terenghi G, Reid Adipose-derived stem cells and nerve regeneration: Promises and pitfalls. Int Rev Neurobiol. 2013;108:121-136
- Vaienti L, Gazzola R, Villani F, Parodi Perineural fat grafting in the treatment of painful neuromas. Techniques in hand & upper extremity surgery. 2012;16:52-55
- Marangi GF, Pallara T, Cagli B, Schena E, Giurazza F, Faiella E, Zobel BB, Persichetti Treatment of early-stage pressure ulcers by using autologous adipose tissue grafts. Plastic Surgery International. 2014;2014
- Lolli P, Malleo G, Rigotti Treatment of chronic anal fissures and associated stenosis by autologous adipose tissue transplant: A pilot study. Diseases of the Colon & Rectum. 2010;53:460-466
- Cantarella G, Baracca G, Forti S, Gaffuri M, Mazzola Outcomes of structural fat grafting for paralytic and non-paralytic dysphonia. Acta Otorhinolaryngologica Italica. 2011;31:154
- DeFatta RA, DeFatta RJ, Sataloff Laryngeal lipotransfer: Review of a 14-year experience. Journal of Voice. 2013;27:512-515
- Sataloff Autologous fat implantation for vocal fold scar. Current opinion in otolaryngology & head and neck surgery. 2010;18:503-506
- Cantarella G, Mazzola RF, Mantovani M, Baracca G, Pignataro Treatment of velopharyngeal insufficiency by pharyngeal and velar fat injections. Otolaryngology– Head and Neck Surgery. 2011;145:401-403
- Papa N, Luca G, Sambataro D, Zaccara E, Maglione W, Gabrielli A, Fraticelli P, Moroncini G, Beretta L, Santaniello A. Regional implantation of autologous adipose tissue-derived cells induces a prompt healing of long-lasting indolent digital ulcers in patients with systemic sclerosis. Cell transplantation. 2014
- Hovius SE, Kan HJ, Smit X, Selles RW, Cardoso E, Khouri Extensive percutaneous aponeurotomy and lipografting: A new treatment for dupuytren disease. Plastic and reconstructive surgery. 2011;128:221-228
- Verhoekx JS, Mudera V, Walbeehm ET, Hovius Adipose-derived stem cells inhibit the contractile myofibroblast in dupuytren’s disease. Plastic and reconstructive surgery. 2013;132:1139-1148
- Bank J, Fuller SM, Henry GI, Zachary Fat grafting to the hand in patients with raynaud phenomenon: A novel therapeutic modality. Plastic and reconstructive surgery. 2014;133:1109-1118
- Damgaard OE, Siemssen Lipografted tenolysis. Journal of Plastic, Reconstructive & Aesthetic Surgery. 2010;63:e637-e638
- Colonna M, Scarcella M, d’Alcontres F, Delia G, Lupo Should fat graft be recommended in tendon scar treatment? Considerations on three cases (two feet and a severe burned hand). European review for medical and pharmacological sciences. 2014;18:753-759
- Merikanto JE, Alhopuro S, Ritsilä Free fat transplant prevents osseous reunion of skull defects: A new approach in the treatment of craniosynostosis. Scandinavian Journal of Plastic and Reconstructive Surgery and Hand Surgery. 1987;21:183-188
- Mojallal A, Lequeux C, Shipkov C, Breton P, Foyatier J-L, Braye F, Damour Improvement of skin quality after fat grafting: Clinical observation and an animal study. Plastic and reconstructive surgery. 2009;124:765-774
- Lockwood Superficial fascial system (sfs) of the trunk and extremities: A new concept. Plastic and reconstructive surgery. 1991;87:1009-1018
- Song AY, Askari M, Azemi E, Alber S, Hurwitz DJ, Marra KG, Shestak KC, Debski R, Rubin Biomechanical properties of the superficial fascial system. Aesthetic Surgery Journal. 2006;26:395-403
- Flynn The use of decellularized adipose tissue to provide an inductive microenvironment for the adipogenic differentiation of human adipose-derived stem cells. Biomaterials. 2010;31:4715-4724
- Brown BN, Freund JM, Han L, Rubin JP, Reing JE, Jeffries EM, Wolf MT, Tottey S, Barnes CA, Ratner Comparison of three methods for the derivation of a biologic scaffold composed of adipose tissue extracellular matrix. Tissue Engineering Part C: Methods. 2011;17:411-421
- Wu I, Nahas Z, Kimmerling KA, Rosson GD, Elisseeff An injectable adipose matrix for soft tissue reconstruction. Plastic and reconstructive surgery. 2012;129:1247
- Omidi E, Fuetterer L, Mousavi SR, Armstrong RC, Flynn LE, Samani Characterization and assessment of hyperelastic and elastic properties of decellularized human adipose tissues. Journal of biomechanics. 2014;47:3657-3663
- Wang L, Johnson JA, Zhang Q, Beahm Combining decellularized human adipose tissue extracellular matrix and adipose-derived stem cells for adipose tissue engineering. Acta biomaterialia. 2013;9:8921-8931
- Healy C, Allen Sr The evolution of perforator flap breast reconstruction: Twenty years after the first diep flap. Journal of reconstructive microsurgery. 2014;30:121-125
- LoTempio MM, Allen Breast reconstruction with sgap and igap flaps. Plastic and reconstructive surgery. 2010;126:393-401
- Erić M, Mihić N, Krivokuća Breast reconstruction following mastectomy; patient’s satisfaction. Acta Chir Belg. 2009;109:159-166
- Diaz-Flores L, Gutierrez R, Lizartza K, et Behavior of In Situ Human Native Adipose Tissue CD34+ Stromal/Progenitor Cells During Different Stages of Repair. Tissue-Resident CD34+ Stromal Cells as a Source of Myofibroblasts. Anatomical record. 2014.
- Gil-Ortega M, Garidou L, Barreau C, et Native adipose stromal cells egress from adipose tissue in vivo: evidence during lymph node activation. Stem cells. 2013;31(7):1309-20.
- Published in Corporate News / Blog
Breakthrough in scaling up life-changing stem cell production
Scientists from the U.K. and Sweden have discovered a new method of creating human stem cells that could solve the problem of meeting large-scale production needs, allowing researchers to fully realize the potential of stem cells for understanding and treating disease.
Understanding Human Pluripotent Stem Cells
Human pluripotent stem cells are undifferentiated cells that have the unique potential to develop into all the different types of cells in the body. With applications in disease modeling, drug screening, regenerative medicine, and tissue engineering, there is already an enormous demand for these cells. This demand will continue to grow as their use in clinical settings and the pharmaceutical industry increases.
Challenges in Stem Cell Production
However, production of stem cells at the scale required for optimal application in modern research and healthcare has not been feasible because available culture methods are either too expensive or reliant on substances that would not be safe for clinical use in humans.
New Stem Cell Culture Method
The research results, published in Nature Communications in July, describe how the scientific team from The University of Nottingham’s Wolfson Centre for Stem Cells, Tissue Engineering and Modelling at Uppsala University in Sweden and GE Healthcare in Sweden have identified and improved human stem cell culture methods. These improvements could lead to quicker and cheaper large-scale industrial production of human pluripotent stem cells.
Using Inter-Alpha Inhibitor Protein
By using a protein derived from human blood called Inter-alpha inhibitor, the team has grown human pluripotent stem cells in a minimal medium without the need for costly and time-consuming biological substrates. Inter-alpha inhibitor is found in human blood at high concentrations and is currently a by-product of standard drug purification schemes.
Advantages of the New Method
The human serum-derived protein can make stem cells attach to unmodified tissue culture plastic, eliminating the need for coating in defined human pluripotent stem cell culture and improving the survival capabilities of the stem cells in harsh conditions. It is the first stem cell culture method that does not require a pre-treated biological substrate for attachment, making it more cost and time-efficient. This paves the way for easier and cheaper large-scale production.
Potential Impact on Research and Healthcare
Existing methods are time-consuming and make developing human stem cell cultures prohibitively costly. This new method has the potential to save time and money in large-scale and high-throughput cultures, being highly valuable for both basic research and commercial applications.
Future Directions
Researchers now intend to combine Inter-alpha inhibitor protein with an innovative hydrogel technology to improve current methods for controlling cell differentiation and apply it to disease modeling. The discovery will help facilitate research into many diseases, although the focus is currently on understanding rare conditions like Multiple Osteochondroma at the cellular level. The aim is to replicate the 3-dimensional environment that cells experience within the body so that lab-bench biology is more accurate in modeling diseases.
Continuing Research and Collaboration
Pijuan-Galitó has been awarded the Sir Henry Wellcome Postdoctoral Fellowship at Nottingham University for her work on the research. This will enable her to combine Inter-alpha inhibitor with improved synthetic polymers in collaboration with fellow regenerative medicine pioneers Professor Morgan Alexander and Professor Chris Denning. The team plans to further improve on current human stem cell culture by designing an economical and safe method that can be easily translated to large-scale production, delivering billions of stem cells necessary to move cellular therapeutics forward in patient settings.
Publication Details
The study, titled “Human serum-derived protein removes the need for coating in defined human pluripotent stem cell culture,” was published in Nature Communications in July 2016.
- Published in Corporate News / Blog
Purest Liver-like Cells to Date Generated from Induced Pluripotent Stem Cells (iPSCs)
Researchers from the Medical University of South Carolina (MUSC) and the University of Pennsylvania have discovered a new methodology for purifying liver cells generated from induced pluripotent stem cells (iPSCs) that could facilitate progress toward an important clinical goal: treating patients with disease-causing liver mutations by transplanting unmutated liver cells derived from their own stem cells.
Background on Liver Stem Cell Research
This new technique follows previous attempts to generate liver-like cells from stem cells, which have yielded heterogeneous cell populations with little similarity to diseased livers in patients.
The Role of Next Generation Genetic Association Studies Program
The National Heart, Lung, and Blood Institute (NHLBI)’s Next Generation Genetic Association Studies Program (Next Gen) was created to bank stem cell lines sourced from patients in genome-wide association studies (GWAS). The goal of the Next Gen Lipid Conditions sub-section – a collaborative effort between Stephen A. Duncan, Ph.D., chair of regenerative medicine at MUSC, and Daniel J. Rader, M.D., and Edward E. Morrisey, Ph.D., both at the University of Pennsylvania – is to help determine the genetic sources of heart, lung, or blood conditions that also include the liver.
Understanding GWAS Studies
The GWAS studies map the genomes in hundreds of people as a way to look for genetic mutation patterns that differ from the genomes of healthy individuals. As GWAS studies map more genomes, they become more likely to find the correct genetic mutations that cause a disease. Once a panel of suspected mutations is built, stem cells from these individuals can be manipulated in culture dishes to differentiate into any of the body’s cells. The cells can be screened to learn more about the mutations and to test panels of drugs that might ultimately help treat patients harboring a disease.
Challenges in Differentiating iPSCs
Problems arise during the cell manipulation process. For example, iPSCs persistently refuse to mature uniformly into liver-like cells when fed growth factors. Traditionally, antibodies have been used to recognize features of maturity on the surfaces of cells and purify cells that are similar, an approach that has been crucial to stem cell research. However, available antibodies that recognize mature liver cells are scanty and tend to recognize many different kinds of cells. The many types of cells in mixed populations have diverse characteristics that can obscure underlying disease-causing genetic variations, which tend to be subtle.
Introducing Chemo Proteomic Cell Surface Capture (CSC) Technology
Instead of relying on antibodies, Duncan and his team embraced a new technology called chemo proteomic cell surface capture (CSC) technology. CSC technology allowed the researchers to map the most highly produced proteins on the surface of liver cells during the final stages of differentiation of stem cells into liver cells. The most abundant protein was targeted with an antibody labeled with a fluorescent marker and used to sort the mature liver cells from the rest.
Results of the New Purification Method
The procedure was highly successful: The team had a population of highly pure, homogeneous, and mature liver-like cells. Labeled cells had far more similar traits of mature hepatocytes than unlabeled cells. Pluripotent stem cells that had not differentiated were excluded from the group of labeled cells.
Implications for Liver Disease Treatment
“That’s important,” says Duncan. “If you’re wanting to transplant cells into somebody that has liver disease, you really don’t want to be transplanting pluripotent cells because pluripotent cells form tumors called teratocarcinomas.”
Duncan cautioned that transplantation of iPSC-derived liver cells is not yet ready for translation to the clinic, but the technology for sorting homogeneous liver cells can be used now to successfully and accurately model and study disease in the cell culture dish.
Future Directions
“We think that the ability to generate pure populations will get rid of the variability, and therefore really help us combine with GWAS studies to identify allelic variations that are causative of a disease, at least in the liver,” he says.
Publication Details
Researchers at the University of Minnesota (Minneapolis) and the Medical College of Wisconsin (Milwaukee) contributed to the study, published August 25, in Stem Cell Reports.=
- Published in Corporate News / Blog
Texas Man Becomes First Adult in the U.S. to Receive Updated Stem Cell Transplant to Treat Leukemia
Introduction to the Groundbreaking Stem Cell Transplant
Chuck Dandridge, a Mansfield, Texas resident, became the first adult in the U.S. to receive a newly modified stem cell transplant that uses genetically engineered blood cells from a family member. The milestone was announced by researchers at UT Southwestern Medical Center’s Harold C. Simmons Comprehensive Cancer Center in Dallas, where the procedure was performed.
Dandridge’s Medical Journey and Diagnosis
Dandridge’s medical journey began in 2013, with a routine doctor’s visit to check his cholesterol levels; lab tests revealed low blood counts and further testing confirmed Dandridge’s diagnosis of myelodysplastic syndrome, also called pre-leukemia or MDS. By 2014, the leukemia had progressed to acute myeloid leukemia (AML), which, according to the National Cancer Institute, affects more than 20,000 Americans annually.
Genetic Testing and Clinical Trials

Dandridge was referred to UT Southwestern’s Simmons Cancer Center, where his leukemia was tested for genetic mutations.
“We wanted to know whether he had specific mutations in his cancer cells,” says Madhuri Vusirikala, M.D., Professor of Internal Medicine and the primary investigator of many UT Southwestern clinical trials related to bone marrow transplantation. “We found a mutation called IDH 2, which causes the body to produce an abnormal protein that promotes excessive cell growth. If you can target that mutation and stop the abnormal protein from being produced, then cells start behaving normally.”
Participation in the AG-221 Clinical Trial
Dandridge enrolled in a UT Southwestern clinical trial for a therapy called AG-221. He took four pills each morning for the next eight months. During that time, Dandridge saw marked improvement although he did not go into complete remission, according to Vusirikala. That success made him eligible for a potentially curative stem cell transplant. But finding a donor proved challenging.
Challenges in Finding a Suitable Donor
“The best chance of finding a full match is usually a full sibling; however, Chuck has no full siblings,” Vusirikala says. Additionally, Dandridge is African American, and minorities are under-represented in the National Marrow Donor Registry—about 70 percent of registry donors are Caucasian. The search for an unrelated donor was unsuccessful. Vusirikala says that he knew Dandridge’s daughter and his son would be at least a half match. Since using a same-sex donor is preferred, as it reduces the risk of complications, his son Jon, 31, emerged as the best choice. But the risk of graft-versus-host-disease (GvHD) following a transplant using a half-match is very high, so they needed a better way to deal with the GvHD risk.
Innovative BP-001 Clinical Trial

Once again, Mr. Dandridge volunteered for a cutting-edge clinical trial, known as BP-001, which processed the stem cells used in the transplant to reduce the risk of rejection and engineered blood cells that can be targeted if GvHD develops after the transplant. The processes being tested in BP-001 are in clinical development by Houston-based Bellicum Pharmaceuticals. The study is evaluating patients with blood cell cancers who have a peripheral blood stem cell transplant from a partially matched relative. Immune cells (T cells) from the related donor are separated from the rest of the stem cells and genetically engineered in the Bellicum laboratory, and then given to the patient along with the stem cell transplant.
Procedure and Outcome of the Transplant
These engineered T cells are modified to include a suicide gene with the help of a retrovirus. If the patient develops GvHD after transplant, the side-effect can be treated by giving a drug called rimiducid to activate the suicide gene and cause the activated GvHD-causing cells to be eliminated. The stem cells given for the transplant were also processed prior to giving them back to Dandridge to reduce the risk of graft rejection as well as GvHD. The genetically engineered blood cells were transplanted from Dandrige’s son, Jon, 31, to the father in three, two-hour infusions at William P. Clements Jr. University Hospital in July 2015, and today the elder Mr. Dandridge’s leukemia is in remission. His immune system is recovering, and the former Norman, Oklahoma YMCA CEO is now mentoring first-time CEOs for the YMCA.
- Published in Corporate News / Blog
Insulin-producing Stem Cells Grown in the Lab Mark a New Era in Stem Cell Therapies for Diabetes
Introduction to Insulin-Producing Pancreatic Beta Cells
A new discovery by researchers on how to activate lab-grown beta cells to mature into functioning cells that produce and release insulin in response to glucose takes a significant step toward a cell therapy treatment for diabetes. Difficulties in manipulating beta cells derived from human stem cells to mature beyond the precursor stage into fully functioning insulin releasers have been an ongoing challenge for researchers.
Breakthrough by Salk Institute Researchers
However, researchers from the Salk Institute for Biological Studies and a team of researchers have achieved this goal with lab-grown beta cells by activating a protein called estrogen-related receptor γ (ERRγ). Their study findings were recently published in the journal Cell Metabolism.
The Role of Human Pluripotent Stem Cells (hPSCs)
Ronald Evans, senior author of the study titled, “ERRγ Is Required for the Metabolic Maturation of Therapeutically Functional Glucose-Responsive β Cells,” explains the self-renewing capacity of human pluripotent stem cells (hPSCs) and their ability to differentiate into most cell types—from neurons to skin cells, to muscle cells, and insulin-producing pancreatic beta cells—has inspired many research teams to find ways to make glucose-responsive beta cells in the lab. Evans and his research team discovered the answer to the insulin-releasing cell conundrum, and summed it up thusly: “In a dish, with this one switch, it’s possible to produce a functional human beta cell that’s responding almost as well as the natural thing.”
Challenges in Lab-Grown Pancreatic Beta Cells
Evans, a molecular biologist at the Salk Institute, says that to create the different types of cells in the lab, researchers coax the pluripotent stem cells (hPSCs) down the various branching paths that fetal cells normally travel in order to differentiate into the various cell types. However, he explains there are many developmental points in this process, and in the case of lab-grown pancreatic beta cells, research kept getting stuck at an early stage.
Role of ERRγ in Adult Beta Cells
In order to determine what might trigger the next step in getting the cells to mature, the researchers compared transcriptomes of adult and fetal beta cells. The transcriptome contains, among other things, the full catalog of molecules that switch genes on and off in the genome, which led them to discover that the nuclear receptor protein ERRγ was more abundant in adult beta cells. The team was already familiar with the protein’s role in muscle cells and had studied its ability to enhance endurance running. Evans says that in muscles, the protein promotes greater growth of mitochondria—the power generators inside cells that accelerate the burning of sugars and fats to make energy.
Surprising Findings on Beta Cells
“It was a little bit of a surprise to see that beta cells produce a high level of this regulator,” Evans says. “But beta cells have to release massive amounts of insulin quickly to control sugar levels. It’s a very energy-intensive process.” The research team then decided to run some tests to look more closely at what role ERRγ might play in insulin-producing beta cells.
A New Era in Creating Functional, Insulin-Producing Beta Cells

After they genetically engineered a deficiency of ERRγ in mice, the researchers found the animals’ beta cells did not produce insulin in response to spikes in blood sugar. Next, they tried to get beta cells made from hPSCs to produce more ERRγ, and it worked! The cells in culture began to respond to glucose and release insulin. Finally, the team transplanted the lab-grown insulin-producing beta cells into diabetic mice and found that from day one, the cells produced insulin in response to glucose spikes in the animals’ blood.
Future Implications and Research
Evans and the research team were justifiably excited by the results. It appears that just switching on the ERRγ protein is sufficient to get the lab-grown beta cells to mature and produce insulin in response to glucose – both in cultures and in live animals. Speculating on the implications of their findings, Evans suggests that when a fetus is developing, because it gets a steady supply of glucose from the mother, it does not need to produce insulin to regulate its blood sugar, so the switch is inactive. But, when the baby is born and takes its first breath and takes in oxygen, this activates the switch. Previous lab attempts to produce beta cells got stuck at the fetal stage. The Salk Institute researchers discovered how to take it to the adult stage, using the same protein that is switched on in nature.
Conclusion
“I believe this work transitions us to a new era in creating functional beta cells at will,” Evans says. He and his research team now plan to examine how the switch might work in more complex models of diabetes treatments. The Salk Institute study precedes another study reported by Medical News Today in which researchers generated mini-stomachs that produce insulin when transplanted into mice.
- Published in Corporate News / Blog
Amazing Stem Cell Research Breakthroughs You Never Heard of
Introduction to Skin Stem Cell Research
Stem cell research has uncovered numerous groundbreaking discoveries over the years, many of which remain relatively unknown. This article highlights one such discovery related to skin stem cells and their critical role in regeneration and maintenance.
Discovery of Dnmt3a and Dnmt3b Proteins
In a significant 2008 study published in “Cell Stem Cell,” researchers from the Catalan Institution for Research and Advanced Studies (CREA) identified two proteins—Dnmt3a and Dnmt3b—that play a crucial role in maintaining skin stem cells. Led by Salvador Aznar Benitah at the Institute for Research in Biomedicine (IRB Barcelona), the study revealed that these proteins are essential for the activation and preservation of skin stem cells.
Function of Dnmt3a and Dnmt3b in Skin Stem Cells

According to Benitah, head of the Stem Cells and Cancer lab at IRB Barcelona, without Dnmt3a and Dnmt3b, skin stem cells fail to activate and eventually diminish within the tissue. The proteins operate primarily on gene enhancers and super-enhancers, facilitating the expression of approximately 1,000 genes critical for the self-renewal of skin stem cells.
Genomic Insights and Mechanisms
Lorenzo Rinaldi, a researcher involved in the study, utilized advanced sequencing techniques to map the genomic distribution of Dnmt3a and Dnmt3b. This revealed their unexpected role in enhancing gene expression through DNA methylation, contrary to their previously known function in gene repression.
Link to Cancer Research
The study also highlighted implications for cancer research, noting that Dnmt3a and Dnmt3b are altered in various types of tumors, including leukemia, lung cancer, and colon cancer. The proteins’ role in DNA methylation and gene regulation suggests potential contributions to tumor development, warranting further investigation in cancer cell models.
Funding and Support
Funded by the Spanish Ministry of Economy and Competitiveness and supported by several foundations and councils, including The European Council for Research (ERC) and the Fundació Marató de TV3, Benitah’s research underscores the importance of public and private partnerships in advancing stem cell and cancer research.
Conclusion
This study represents a significant advancement in understanding the molecular mechanisms governing skin stem cell maintenance and its implications for both regenerative medicine and cancer biology. Continued research into Dnmt3a and Dnmt3b promises to unveil new therapeutic strategies and insights into cellular regeneration and disease progression.
- Published in Corporate News / Blog
New Guidelines for Stem Cell Research and Therapies Aim to Protect Patients from Charlatan Quackery
Introduction
Stem cell research has advanced significantly, leading to a myriad of treatment options. However, the field faces challenges from unscrupulous providers and premature publicity.
Professional Guidelines for Responsible Stem Cell Research
International Society for Stem Cell Research (ISSCR)

The ISSCR leads in setting high standards for translational stem cell research:
- Emphasizes rigorous preclinical evidence and peer review.
- Highlights the importance of IRB review and comprehensive informed consent.
International Society for Cellular Therapy (ISCT)
The ISCT expands its scope beyond stem cells, advocating for broader cell-based interventions:
- Focuses on defining scientific evidence and regulatory practices.
- Addresses implications across clinical practice and commercialization.
Development of New Guidelines
Terminology and Scientific Evidence
Efforts are underway to standardize terminology and define scientific evidence levels critical for ethical and effective stem cell therapy.
ISSCR’s 2016 Guidelines Update
In 2016, ISSCR updated guidelines cover:
- Emerging technologies like gene editing and induced pluripotent stem cells (iPSCs).
- Upholding ethical standards such as the “14-day rule” for embryo experimentation.
Key Topics Addressed in the Revised Guidelines
The updated guidelines include:
- Oversight processes for embryo research and mitochondrial replacement therapy.
- Standards for preclinical and clinical research, emphasizing safety and efficacy.

Advancements in Stem Cell Research
Stem cell therapies show promise in treating a range of conditions, leveraging pluripotent stem cells for tissue repair and genetic disease treatments.
Conclusion
Stem cell research continues to evolve responsibly, offering hope for future medical advancements while safeguarding patient interests against fraudulent practices.
- Published in Corporate News / Blog
Researchers Move Closer to Lung Stem Cell Therapies to Treat Chronic Lung Diseases
Introduction
Chronic lung diseases, including COPD, bronchitis, emphysema, and asthma, are significant causes of mortality in the U.S., highlighting the urgent need for advanced treatments.
Stem Cells in the Lung
Types and Functions of Lung Stem Cells
Human lungs are complex organs comprising:
- Conducting Airway Tubes: Includes trachea, bronchi, and bronchioles.
- Gas Exchange Regions: Alveolar spaces crucial for oxygen exchange.
Role of Progenitor Cells
Progenitor cells like tracheal basal cells and alveolar type 2 cells play a vital role in maintaining lung health by replacing old or damaged cells.
Diversity of Lung Stem Cells
Embryonic and adult lung stem cells contribute differently:
- Research indicates their role in lung development and regeneration, with potential implications for disease treatment.
Current Research on Lung Stem Cell Therapies
Adult Mesenchymal Stem Cells (hMSCs)
hMSCs are pivotal in:
- Immunomodulation: Regulating immune functions and secreting bioactive molecules for anti-inflammatory and regenerative effects.
- Versatility: Capable of generating various cell types, potentially aiding in lung tissue repair.
Insights into Lung Disease Causes
Understanding lung stem cell biology enhances knowledge of disease mechanisms like COPD, paving the way for innovative treatments.

Future Prospects of Lung Stem Cell Therapies
Translational Research and Clinical Applications
Ongoing studies aim to:
- Identify and characterize lung stem cells in humans, advancing potential clinical applications.
- Explore personalized medicine approaches using lung stem cells for targeted therapies.
Conclusion
Progress in lung stem cell research holds promise for developing effective therapies to combat chronic lung diseases, offering hope for improved patient outcomes and quality of life.
- Published in Corporate News / Blog
The History of Research on Adult Stem Cells: We’ve Come a Long Way
Introduction to Adult Stem Cells
Adult stem cells, also known as somatic stem cells, are undifferentiated cells found among differentiated cells in tissues or organs. They play a crucial role in tissue maintenance and repair.
Types and Functions of Adult Stem Cells
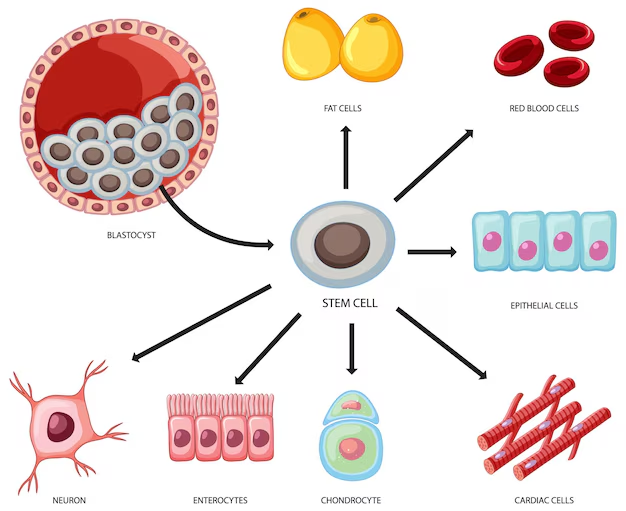
Bone Marrow Stem Cells
- Hematopoietic Stem Cells: Responsible for forming all blood cell types.
- Mesenchymal Stem Cells: Can differentiate into bone, cartilage, fat cells, and support blood formation.
Brain and Heart Stem Cells
Recent discoveries have identified stem cells in unexpected locations like the brain and heart, challenging previous beliefs and expanding potential applications in transplantation therapies.
Historical Development of Adult Stem Cell Research
Early Discoveries
In the 1950s, researchers identified hematopoietic stem cells in bone marrow, marking the beginning of significant research into adult stem cells.
Advances Over Decades
- 1960s: Discovery of neural stem cells in the brain.
- 1990s: Confirmation of adult brain’s capability to generate neurons and other cell types.
Distribution of Adult Stem Cells in the Body

Adult stem cells are found in various organs and tissues, residing in specific niches critical for their function and activation in response to tissue repair needs or disease.
Methods to Identify Adult Stem Cells
Scientists employ several techniques:
- Labeling and Differentiation: Using molecular markers to track specialized cell types generated.
- Transplantation Studies: Removing and labeling cells, then transplanting them to observe tissue repopulation.
Future Directions in Adult Stem Cell Research
Ongoing research aims to:
- Further characterize and manipulate adult stem cells for therapeutic purposes.
- Explore personalized medicine applications using stem cell technologies.
Conclusion
The study of adult stem cells has evolved significantly, offering promising avenues for understanding and treating various diseases. Continued research holds potential for transformative advancements in regenerative medicine.
- Published in Corporate News / Blog